I COULD DANCE.... BEFORE THE FALL
TRAPPED BY THE FALL: CHAPTER THREE
Physiotherapy, motivation, and reclaiming independence after trauma
Trapped by the Fall | Chapter 3: I Could Dance… Before the Fall
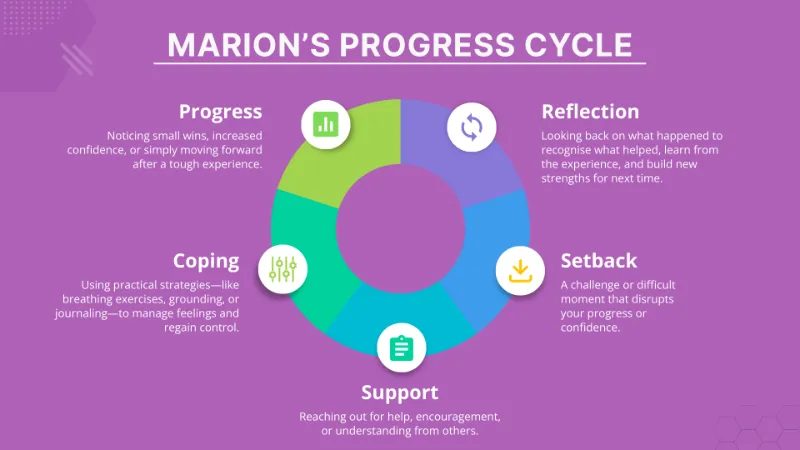
After navigating shrinking routines and the early steps of recovery, Chapter Three focuses on identity, movement, and how setbacks and support shape the healing process.


From Wheelchair to Movement
Her physiotherapy sessions became a daily test of courage. Simple exercises, such as lifting a leg, balancing, or walking a few steps, were accompanied by a rapid heartbeat and the persistent thought: “What if I fall again?”
Building on the small steps described in Chapters One and Two, Marion’s journey now focused on regaining independence and rediscovering her identity.
Marion began her recovery in a wheelchair, facing the reality that independence felt far away. For the first several weeks, she relied on her wheelchair to get around, gradually building up enough strength to stand and walk short distances.
Progress was slow and physically demanding, but she committed herself fully to physiotherapy. Alongside standard treatment, she undertook private hydrotherapy sessions, using the support of water to rebuild strength, balance, and confidence in movement.
A typical hydrotherapy session involved gentle walking, balance exercises, and learning to trust her body in a safe environment—sometimes just standing in the water and noticing how her muscles responded. These sessions helped Marion feel less afraid of movement and made each small gain seem possible.
Each session required persistence.
Hospital Experience and Psychological Impact
Marion also speaks candidly about her time in the hospital, describing feelings of frustration, abandonment, and anger. She recalls, “Twice I was left. Nobody remembered me in the corner, and I’m not a quiet person.” These types of negative hospital experiences are unfortunately common, and it is natural to feel upset or discouraged when they happen.
If you are not sure what to say, using a simple phrase or question can help you start:
- " Excuse me, could you please help me understand what is happening with my care? "
- " I am feeling anxious right now. Can someone check in on me or explain what comes next? "
- " Can I Speak to someone about my worries or feelings? "
- " I need some support. Is there a nurse or advocate I can talk to? "
- " I'm not sure what to exect next. Could you talk me through it? "
- " Can you tell me who to ask if I need something or don't understand what is happening? "
These simple scripts help break the ice and make it easier to express your needs or concerns to the medical team. Remember, you have the right to ask questions and to receive care that feels respectful and supportive.
Seeking support from friends, family, or hospital support services can also help you feel less alone and more empowered during challenging times. These experiences had a lasting emotional impact, shaping how she dealt with rehabilitation and reinforcing feelings of uncertainty and dread.
Understanding Anxiety and Regaining Control
Working with her psychologist, Marion started understanding how anxiety can influence recovery. Fear of falling, pain, or failure often disrupted her progress, even when her body was physically capable.
- – Writing down her worries before a session
- – Practising controlled breathing and visualisation
- – Celebrating each milestone, no matter how small
Through cognitive therapy, relaxation techniques, and confronting negative thought patterns, she learned to regain control over her responses.

With therapy, family support, and determination, Marion began reconnecting with the person she had been before the fall. Alongside her family, encouragement from friends and members of a local support group also played a key role, giving reassurance and understanding from those who had encountered similar challenges.
Seeking out support groups or connecting with others who share similar experiences can make a real difference, helping to diminish feelings of isolation and reminding you that you are not alone in your journey.
If you are not sure where to start, two places to consider are Shout (text SHOUT to 85258 for confidential mental health support in the UK, available 24/7) or Mind’s Side by Side online community, which allows people affected by mental health difficulties to share experiences and find peer support.
You might also look for recovery and trauma forums or communities online, reach out to local charities or organisations that support people in similar situations, or ask your healthcare provider for recommendations. Many communities have social media groups or listings on clinic and library notice boards that can point you towards peer support options.
Sometimes, taking the first small step to reach out—even joining an online conversation or sending a message—can help you feel more connected.
Reflective Takeaway
UK Support Resources:
- Samaritans: 116 123 (free, 24/7 helpline) – For anyone struggling to cope, feeling low, or needing someone to talk to.
samaritans.org - Shout: Text ‘SHOUT’ to 85258 (free, 24/7 text support) – Confidential mental health support via text.
giveusashout.org - Student Minds: Mental wellness resources and help for students.
studentminds.org.uk - Switchboard (LGBTQ+): 0300 330 0630 – For LGBTQ+ support.
switchboard.lgbt - LGBT Foundation: 0345 3 30 30 30 – Advice and support for LGBTQ+ people.
lgbt.foundation - Galop: 0800 999 5428 – For LGBTQ+ people experiencing abuse or hate crime.
galop.org.ukFor a full list of resources, please see the final page of this series.
© 2025 All Rights Reserved.
